

The Current Landscape of 3D Printingin Endovascular Intervention
Jasamine Coles-Black1,2, Jason Chuen1,2
1.Austin Health 3D Medical Printing Laboratory, Austin Health,The University of Melbourne
2.Department of Vascular Surgery, Austin Health, The Universityof Melbourne
3D printing has begun to establish itself as a useful adjunct inVascular Surgery, where the ability to visualise complex anatomywith physical 3D models provides better anatomical clarity than 3Dreconstructions or 2D imaging modalities. Of note is its increasingutility as an interventional planning tool for endovascularprocedures. Our review presents a broad range of applications onhow 3D printing is facilitating endovascular approaches, includingmodels for preoperative planning, education and simulation.
Conclusion
3D printing is fast becoming an established practice in VascularSurgery units worldwide. Many units, including our own, arestarting to explore the applications of 3D printing in endovascularintervention, in addition to within Vascular Surgery as a whole.We attest to the enormous potential for growth in this field, andthe ease of adoption of this new technology.
Method
Results
A literature search was performed in July 2017 using OvidMEDLINE, Ovid EMBASE and PubMed using PRISMAguidelines. The search terms used were “Printing, Three-Dimensional” AND “Vascular Surgery” AND “Endovascular”. Thisresulted in 18 articles, which were independently read in full toidentify relevant studies. The findings from these studies werethen compared against our own centre’s experiences with thetechnology.
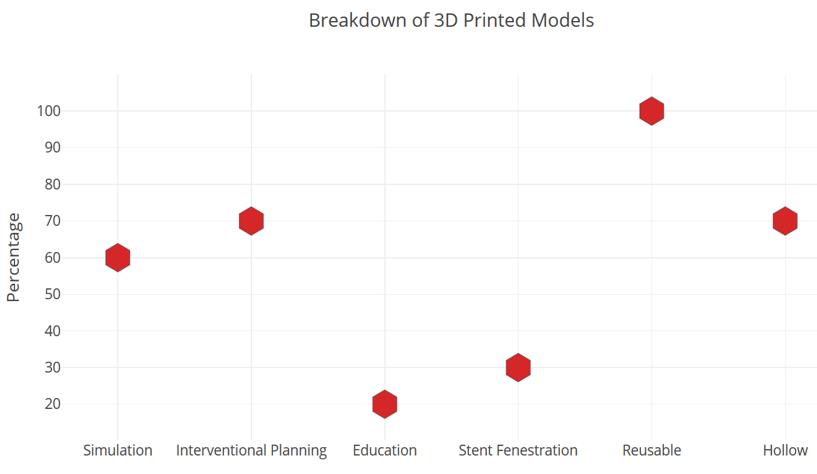
Our literature search identified 10 publications reporting on theuse of 3D printing in endovascular procedures, of which 3 (30%)related to the planning of fenestrated grafts. In 6 (60%) of thearticles, the 3D printed models were used for simulation. Thevast majority (80%) of articles utilised the 3D printed models forinterventional planning. In keeping with this, 70% of publicationsdetailed the creation of hollow models, facilitating proceduralrehearsal. In addition, in 100% of cases, the 3D printed modelsdeveloped for the studies did not degrade after simulation ormanual interrogation. Despite this, only 3 (30%) of articlesinvolved the use of 3D printed models for trainee education.Therefore, we highlight the largely untapped potential for thesemodels to be reused for trainee education, which was notexplored in the majority of articles.
The studies’ conclusions correlate with our own experiences inour 3D printing lab, where expert vascular surgeons havedeemed 3D printed models valuable in the planning of complexcases, such as in cases with short or very angulated necks, orfor the planning of fenestrations in juxtarenal aneurysms.



@3DMedLab


Introduction
